The information below is based on the paper: “Detection of Subclinical Keratoconus With a Validated Alternative Method to Corneal Densitometry” by Alejandra Consejo; Marta Jiménez-García; Ikram Issarti & Jos J. Rozema.
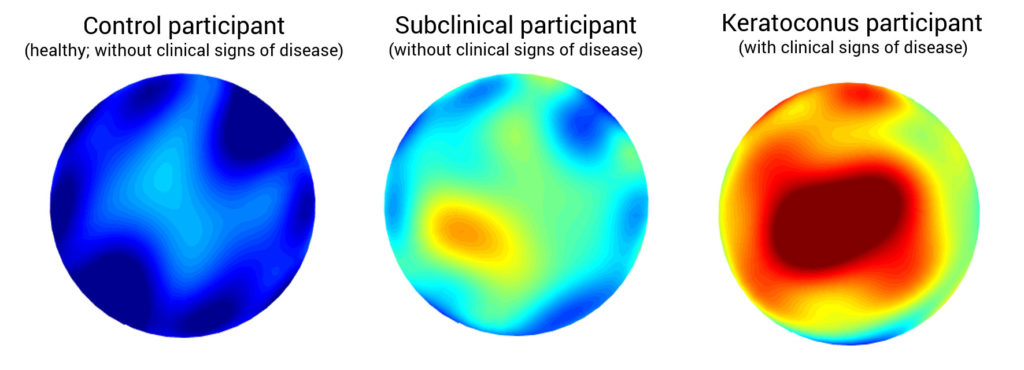
Keratoconus is an eye disease that affects the cornea, the clear transparent lens outside our eyes. Keratoconus is a progressive disease that affects 1 in 1000 people and, if untreated, might lead to blindness. However, the early detection of keratoconus is still a clinical challenge.
This work was developed in the frame of MAiCRO project, financed by National Science Center, at ICTER in collaboration with colleagues from Volantis, from the Antwerp University Hospital in Belgium.
In this paper a reinterpretation of already available clinical data to enhance the early detection of keratoconus is proposed. During a standard ophthalmologist examination, doctors focus mainly on analyzing macroscopic data: corneal shape, thickness, radius, and other geometrical parameters. The analysis of this information allows the ophthalmologists to diagnose different eye diseases, but it has repeatedly proven to be not enough for a proper diagnosis, specially in the early cases.
What innovation brings the approach proposed by Consejo, Jiménez-García, Issarti & Rozema? The authors define a diagnostic tool based not only on traditional macroscopic parameters, but also on microscopic data of the cornea’s tissue, combining both approaches (macro- and microscopic information) in a methodology denominated MAiCRO. In particular, in this article, corneal tomographies of sixty right eyes were obtained from the Department of Ophthalmology at the Antwerp University Hospital. The patients were divided in three study groups: controls (20 eyes), clinical keratoconus (20 eyes), and subclinical keratoconus (20 eyes) – subclinical keratoconus are eyes that have not developed the disease yet. The study defined biomarkers that account for tissue transparency and compared these biomarkers between study groups. To define those biomarkers different techniques of image processing and statistical modelling of light intensity distribution (in other words, using information of the journey of the light through the cornea) were applied.
The results of the study validated with a ROC analysis confirmed a discrimination success of 97% when differentiating between subclinical keratoconus and control eyes, which is a much higher clinical diagnosis rate success than clinical standards.
One of the benefits of this methodology is the reinterpretation of commonly available hospital data obtained through non-invasive ophthalmological tomography based on Scheimpflug technology. Using MAiCRO methodology, doctors do not need to take more measurements, or perform additional tests in order to be able to diagnose Keratoconus more effectively than before.
Dr Alejandra Consejo is a Postdoctoral fellow collaborating with ICTER.
Supported by funding from the National Science Centre (Poland) under the OPUS 19 funding scheme (project no. 2020/37/B/ST7/00559).